P Shot UK vs Penile Implants: Non-Surgical vs Surgical Options for Erectile and Sexual Dysfunction

Erectile dysfunction (ED) affects a significant proportion of men in the United Kingdom. NHS estimates indicate that approximately 50% of men aged between 40 and 70 experience some degree of erectile difficulty during their lifetime. As awareness grows and stigma declines, more men now seek evidence-informed treatment options beyond conventional pharmacological therapies.
Two treatments appear with increasing frequency in clinical and patient-facing literature: the P Shot UK(also known as the Priapus Shot or P-shot) and penile implant surgery. These sit at opposite ends of the intervention spectrum. One is a minimally invasive, regenerative injection-based procedure. The other is a permanent surgical implant requiring general or spinal anaesthesia. Any man considering treatment must understand the mechanisms, evidence, risk profiles, and clinical appropriateness of each option.
This article provides a structured, clinically grounded comparison of both to support informed decision-making.
What Is the P Shot?
Overview of the Priapus Shot
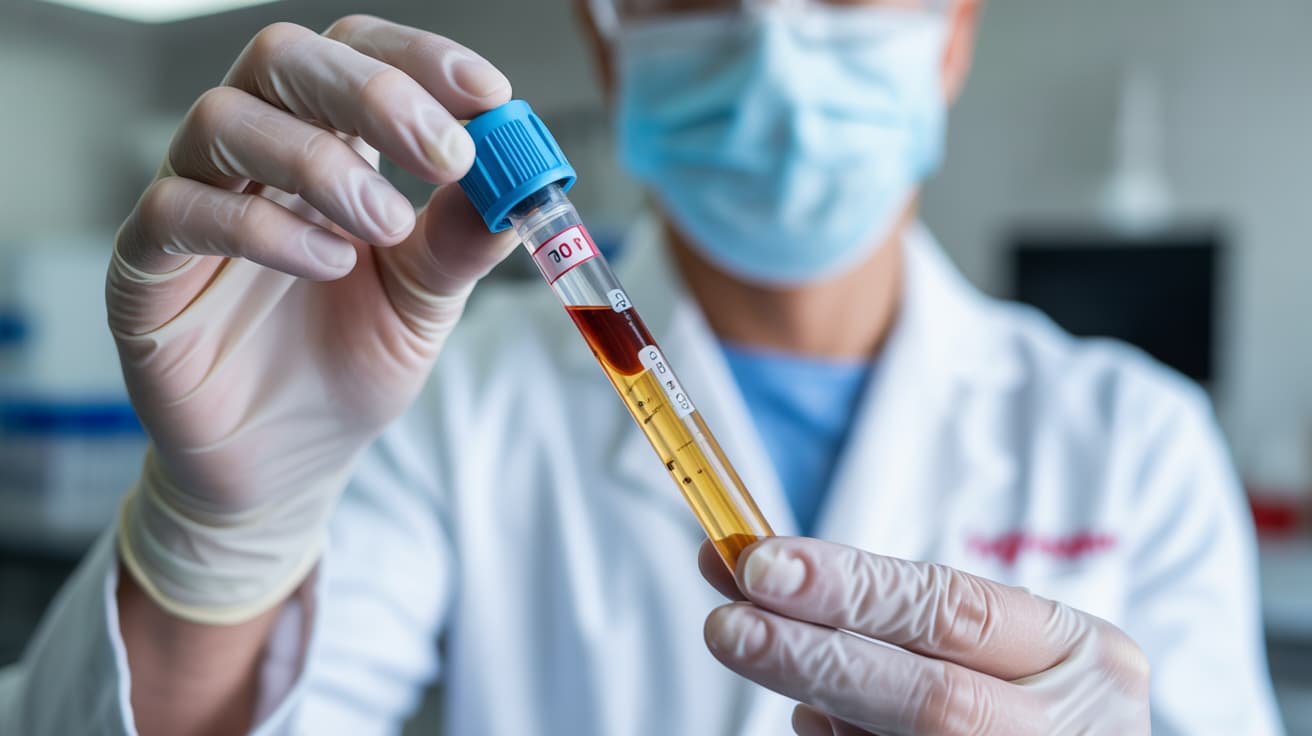
The P Shot, or Priapus Shot, is a non-surgical treatment that uses platelet-rich plasma (PRP) drawn from the patient’s own blood. PRP is a concentrated preparation of platelets and growth factors. A clinician produces it by centrifuging a blood sample taken in clinic. The clinician then injects the resulting plasma into specific anatomical zones of the penis — typically the corpus cavernosum and the glans — to stimulate tissue regeneration and improve vascular function.
The procedure takes approximately 45 to 60 minutes. A clinician performs it under topical or local anaesthesia. It involves no incision, no hospital admission, and no general anaesthetic. Most patients return to daily activities the same day.
The Mechanism Behind PRP Injections
Platelet-rich plasma contains several key growth factors. These include platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), and transforming growth factor-beta (TGF-β). Together, these factors support neovascularisation — the formation of new blood vessels — as well as cellular proliferation and tissue repair.
In the context of erectile function, these processes aim to improve local blood flow. They also work to restore tissue integrity that ageing, diabetes, cardiovascular disease, or prior pelvic surgery may have compromised.
Clinicians already use PRP across multiple specialties, including orthopaedics and dermatology. Its application to male sexual medicine represents a developing area of research.
What Does the Evidence Say?
The evidence base for P shot treatment continues to grow, but it remains at an early stage. Several peer-reviewed studies report positive outcomes in men with mild to moderate erectile dysfunction. These include improvements in erectile function scores — measured using the International Index of Erectile Function (IIEF) — and patient-reported satisfaction.
A 2021 systematic review in Sexual Medicine Reviews examined PRP therapy for erectile dysfunction. The majority of included studies showed statistically significant improvements in erectile function. However, the authors identified key limitations: small sample sizes, an absence of placebo-controlled trials, and variation in injection protocols.
The NHS does not currently commission PRP for erectile dysfunction as a standard treatment. NICE (the National Institute for Health and Care Excellence) has not yet issued formal guidance endorsing it. As a result, clinicians offer it primarily through regulated private medical practice. Men seeking P shot London or elsewhere in the UK should look for practitioners with appropriate medical qualifications and transparent outcome data.
P Shot Before and After: Realistic Expectations

Men reviewing P shot before and after data should hold measured expectations. The procedure does not guarantee a cure for erectile dysfunction. Clinicians also do not recognise it as a method for significant permanent penile enlargement.
Published data and clinical observations point to several potential benefits:
- Improved erectile rigidity and sustainability
- Enhanced penile sensitivity
- Possible modest improvements in penile dimensions through better tissue perfusion
- Improved response to PDE5 inhibitors such as sildenafil in some patients
The phrase penile injection growth appears colloquially in relation to PRP treatment. However, any dimensional changes remain modest. Clinicians do not position dimensional change as a primary aim of the procedure.
Where results occur, they typically become apparent over four to twelve weeks as tissue remodelling progresses. Some men need more than one treatment session.
P Shot Price UK
The priapus shot price varies across the UK. Factors include the clinic, the practitioner’s qualifications, and geographic location. In London, P shot treatment typically costs between £1500 and £2,500 per session. Male enlargement injections cost UK -wide may differ outside London. Patients should request a full cost breakdown. This should cover the consultation, blood draw, PRP preparation, and the injection itself.
What Are Penile Implants?
Overview of Surgical Penile Prostheses
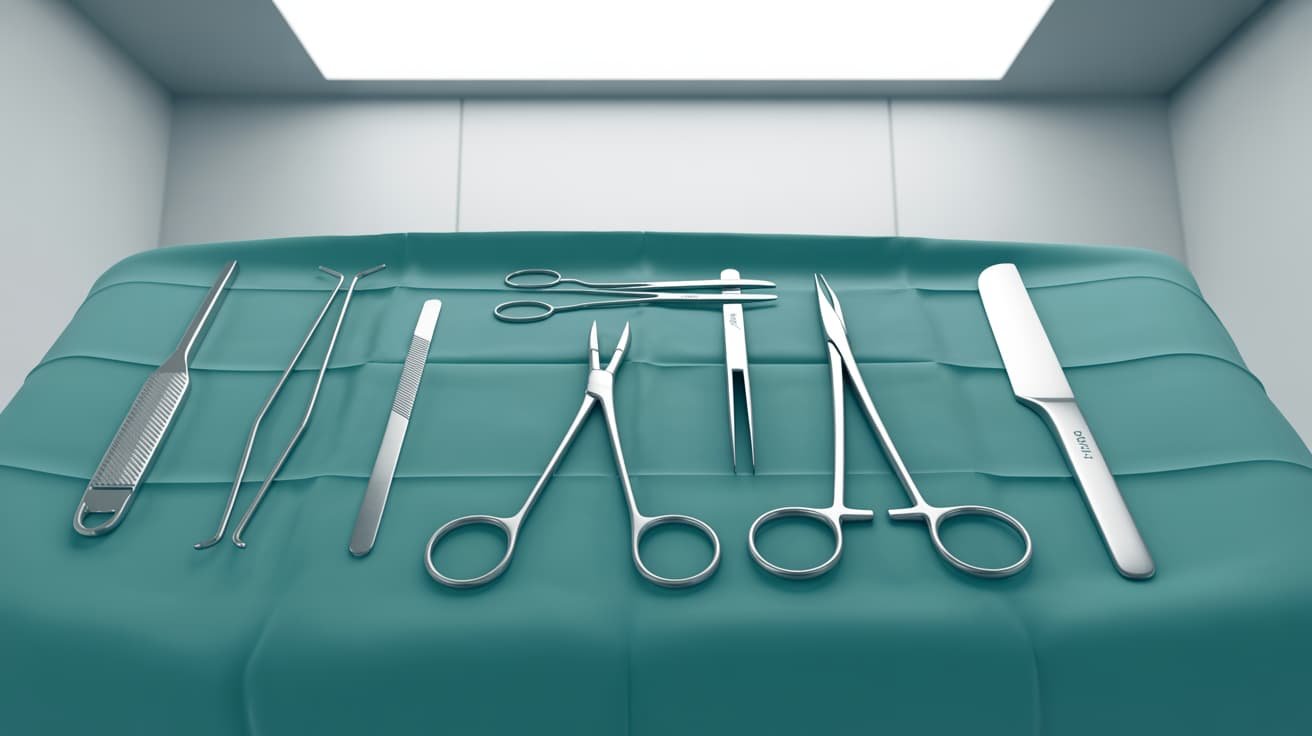
Penile implant surgery — also known as penile prosthesis implantation — involves a surgeon placing a mechanical device inside the penis. This device enables erections on demand. Clinicians consider it a third-line treatment for erectile dysfunction. They typically recommend it after pharmacological and non-invasive treatments have failed.
UK surgeons use two principal types of penile prostheses:
Inflatable (hydraulic) prostheses: A surgeon implants two cylinders in the corpora cavernosa, a fluid reservoir in the abdomen or pelvis, and a pump in the scrotum. The patient activates the pump to move fluid into the cylinders, producing an erection. This is the most commonly implanted type. Studies associate it with higher patient satisfaction rates.
Malleable (semi-rigid) prostheses: A surgeon implants two bendable rods in the corpora cavernosa. The patient manually positions the penis upward for intercourse and bends it downward for concealment. This device is mechanically simpler. Clinicians sometimes prefer it for patients with limited hand dexterity.
Surgical Procedure and Recovery
A surgeon performs the procedure under general or spinal anaesthesia. It typically takes 45 to 90 minutes. The patient requires a hospital admission of one to two nights. Restricted activity follows for four to six weeks. Most patients resume sexual activity after six to eight weeks.
The surgery is irreversible in practical terms. Once a surgeon alters the corpora cavernosa during implantation, natural erections will no longer occur. Patients must clearly understand this before giving consent.
Evidence and Clinical Guidelines
Penile implant surgery has a considerably longer and more robust evidence base than PRP-based treatments. The procedure has been available since the 1970s. Extensive peer-reviewed literature supports its use. Long-term studies report patient satisfaction rates of 85% to 92% for inflatable prostheses. Partner satisfaction rates are similarly high.
NICE has issued guidance on inflatable penile prostheses (IPP). The guidance confirms the procedure as safe and effective for appropriately selected patients. NICE recognises it as an established intervention for refractory erectile dysfunction. The NHS funds penile prosthesis implantation in some clinical circumstances, though availability varies by integrated care board.
Head-to-Head Comparison: P Shot vs Penile Implant
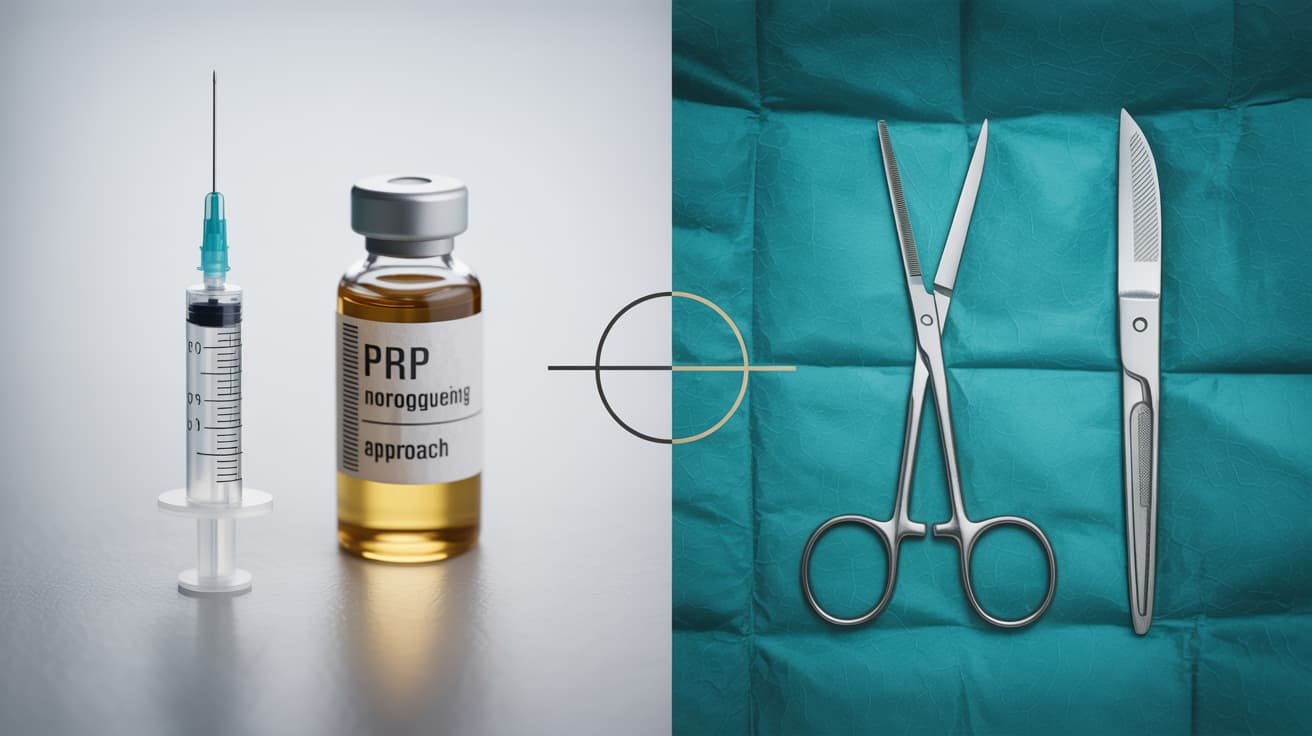
Invasiveness and Recovery
The P-shot is a minimally invasive outpatient procedure. It involves no surgical incision, no general anaesthetic risk, and no hospital stay. The penile implant is a formal surgical procedure. It requires theatre time, anaesthesia, an overnight admission, and several weeks of post-operative recovery.
Men who wish to avoid surgery find that the P shot UK pathway offers a substantially lower-risk starting point.
Reversibility
PRP injections cause no permanent structural change. If outcomes fall short of expectations, no irreversible anatomical alteration has taken place. Penile implant surgery permanently modifies the corpora cavernosa. Surgeons can remove implants, but this carries further surgical risk and potential tissue loss.
Mechanism of Action
PRP therapy targets the body’s own regenerative capacity. It addresses the underlying vascular and tissue pathology that contributes to erectile dysfunction. It does not mechanically produce an erection. Instead, it works to restore physiological function. A penile implant bypasses the natural erectile mechanism entirely. It provides a consistent mechanical erection regardless of psychological or vascular factors.
Suitability
The Pshot or P injection suits men with mild to moderate erectile dysfunction. It also suits men who have responded partially to oral medications, or those seeking a non-surgical adjunct to existing treatments. Men wishing to proactively support penile health may also consider it, though this indication sits outside any formal clinical pathway.
Penile implants suit men with severe, refractory erectile dysfunction. These include men with Peyronie’s disease, post-radical prostatectomy ED, or ED from severe vascular disease. In these cases, less invasive treatments have consistently failed.
Risk Profiles
The P-shot before and after risk profile is low. Studies report minimal adverse effects. These typically include transient bruising, swelling, or mild discomfort at the injection site. Infection and adverse reactions are rare when a qualified clinician performs the procedure under appropriate conditions.
Penile implants carry the full risk profile of surgical procedures. These include infection (in approximately 1–3% of cases), mechanical failure (in less than 5% of inflatable devices at ten years), erosion, and the consequences of device malfunction. Some patients require revision surgery.
Cost Comparison
P shot UK procedures typically cost between £1500 and £2,500 per session at private UK clinics. Clinicians may advise multiple sessions. Penile implant surgery in UK private settings costs considerably more — typically £10,000 to £20,000, depending on device type and surgical centre.
The NHS funds penile implants in some cases. It does not fund PRP treatments.
Clinical Appropriateness and Shared Decision-Making
The Role of the Treating Clinician
Neither treatment suits every patient. Clinicians must individualise the decision between a priapus shot London or other non-surgical PRP approach and surgical prosthesis implantation. A full medical history is essential. The clinician must also assess erectile dysfunction severity using validated instruments such as the IIEF-5, review comorbidities, and discuss patient expectations.
Any man considering either intervention needs assessment by a qualified medical professional. This should be someone who can interpret clinical findings, arrange relevant investigations, and obtain appropriate informed consent — not a non-medically trained practitioner.
At pshots.co.uk, Dr Syed Nadeem Abbas (MBBS, MRCS RCS Edinburgh, MRCGP, MSc Aesthetic Plastic Surgery with Distinction — Queen Mary University London) offers PRP-based treatments within a clinically governed framework on Harley Street, London.
Combination Approaches
Some men benefit from a staged or combined approach. A clinician may use PRP therapy as a first-line intervention or alongside pharmacological treatment. If non-surgical treatments produce insufficient improvement, the clinician can then revisit surgical options. This stepwise approach aligns with principles that sexual medicine guidelines support.
Key Limitations of Current Evidence
The evidence base for P shot treatment — including P shot before and after outcome data — is less mature than that for penile implant surgery. Most PRP studies to date involve small patient cohorts. They also lack long-term follow-up beyond 12 months and do not use randomised controlled trial designs with placebo arms. These gaps limit the strength of conclusions that researchers and clinicians can draw.
Both clinicians and patients should interpret favourable reports with appropriate scientific caution. Researchers need to complete larger multi-centre trials before bodies such as the NHS or NICE can formally recommend PRP-based therapy for erectile dysfunction.
Health Perspective Moving Forward
The choice between a P Shot UK procedure and penile implant surgery reflects more than personal preference. It reflects the severity of the underlying condition, the patient’s medical history, prior treatment responses, and individual values around surgical risk.
The priapus shot is a non-surgical, low-risk, regenerative intervention. It suits men with mild to moderate erectile dysfunction who wish to avoid surgery. Its evidence base continues to develop and has not yet reached the threshold for mainstream NHS endorsement. Nevertheless, it remains a clinically rational option when a qualified practitioner delivers it.
Penile implants offer a well-evidenced, highly effective surgical solution for severe, treatment-refractory erectile dysfunction. They deliver consistent mechanical function and high long-term satisfaction. However, they require patients to accept irreversible anatomical alteration and the inherent risks of surgery.
Informed decision-making demands a thorough consultation, honest communication about realistic outcomes, and a clear understanding of what each intervention can and cannot achieve. No man should pursue either treatment without medical assessment and open discussion of alternatives.
The central question for any man navigating these options is not simply which treatment works — but rather: which treatment is clinically appropriate for this individual, at this stage of their condition, and given their specific circumstances and expectations?
Read more: P Shot Treatment: Procedure Steps, Recovery, Aftercare, and Results Timeline
P Shot London: How to Choose a Safe Clinic and What to Expect at Your Consultation