Priapus Shot London – The Science Behind Platelet-Rich Plasma Therapy

Mark was 47 when he first noticed the changes. Not dramatic ones. Just a gradual erosion of confidence. Erections that were less reliable. Sensation that felt duller than it once did. He had no underlying illness. His blood pressure was fine. Moreover, his testosterone levels sat within normal range. Yet something had clearly shifted.
His GP referred him for general health checks. Everything came back unremarkable. And that, in many ways, made things harder. There was no diagnosis to treat. No pill to prescribe. His GP simply told him that some decline was normal with age.
It was only when Mark started researching that he came across a term he had not heard before: the Priapus Shot London clinics were offering. More specifically, he found articles about platelet-rich plasma therapy applied to penile tissue. He was sceptical at first. But he was curious enough to keep reading.
What the Priapus Shot Actually Is
The Priapus Shot — often abbreviated as the P-shot or Pshot — is a procedure that uses a patient’s own blood to stimulate tissue repair and regeneration. Furthermore, it belongs to a broader category of regenerative medicine that has gained significant traction across multiple specialities over the past two decades.
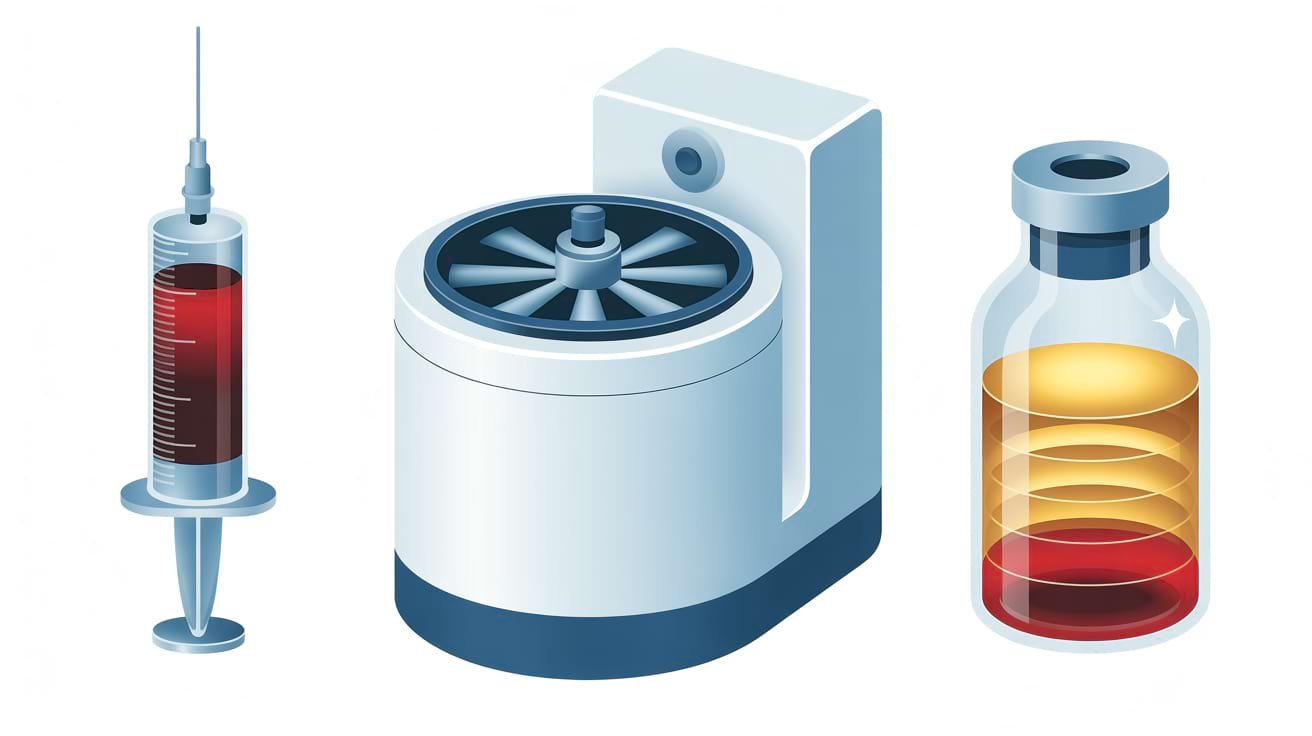
The name comes from Priapus, the Greek god associated with male fertility. Dr Charles Runels developed and trademarked the procedure in the United States. It involves drawing a small amount of the patient’s blood, processing it in a centrifuge to isolate platelet-rich plasma (PRP), and then injecting that concentrated plasma into specific areas of the penis.
The theory is straightforward. Platelets contain growth factors — chemical signals that trigger cellular repair and new blood vessel formation. When a clinician delivers concentrated PRP directly into erectile tissues, those growth factors act locally. As a result, they stimulate angiogenesis (the formation of new blood vessels), encourage collagen remodelling, and potentially support nerve sensitivity.
Crucially, this is not a synthetic drug. It is the patient’s own biology, redirected.
The Biology of PRP: Why It Works in Other Tissues
To understand why P-shot treatment has attracted medical interest, it helps to look at the broader evidence for PRP in regenerative medicine.
Surgeons have used PRP in orthopaedics since the 1980s, applying it to bone grafts and wound healing. Over time, its use expanded to tendon injuries, osteoarthritis, and hair loss treatment. In addition, research published in peer-reviewed journals has consistently demonstrated that concentrated platelets accelerate tissue healing and promote angiogenesis in damaged or poorly vascularised areas.
The mechanism relies largely on growth factors held within alpha granules inside platelets. These include platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), transforming growth factor-beta (TGF-β), and insulin-like growth factor (IGF-1). Each one plays a role in stimulating cell proliferation and tissue remodelling.
When a clinician injects PRP into the corpus cavernosum — the erectile tissue that fills with blood during arousal — these same mechanisms follow. The tissue responds to the growth factors. New capillaries form. Consequently, existing tissue quality may improve.
What the Research Says About Penile Injection Growth
The clinical evidence for the P injection in sexual medicine is still building. It has not yet reached the level of large randomised controlled trials, which is the gold standard framework that NICE (the National Institute for Health and Care Excellence) outlines for evaluating new interventions in the UK. That is an honest and important point to make.
However, several smaller peer-reviewed studies have produced encouraging findings. A 2019 study published in the Journal of Sexual Medicine examined PRP therapy in men with erectile dysfunction and reported statistically significant improvements in erectile function scores at 12 months post-treatment. Similarly, another study looked at men who had experienced erectile changes following prostate cancer treatment — a group that often responds poorly to conventional pharmacological options.
Across these studies, researchers consistently highlight a few key findings. First, the procedure appears well-tolerated with a low adverse event profile. Second, clinicians recorded improvements in erectile function, penile sensitivity, and patient-reported satisfaction. Third, effects tend to appear gradually over six to twelve weeks, which aligns with the biological timeline of angiogenesis and tissue remodelling.
In other words, this is not a quick fix. It is a biological process that unfolds over time.
P-Shot Before and After: What Patients Report
Clinical trial data tells one part of the story. Patient accounts tell another. Neither is sufficient alone, but together they form a more complete picture.
Men who have undergone the P shot before and after comparison often describe changes in three areas. The first is erectile quality — they report firmer, more reliable erections. The second is sensitivity — some describe a return of sensation they felt had diminished over the years. The third is confidence — which, while not a measurable clinical endpoint, has a real impact on sexual function and relationship quality.
Beyond these core changes, a proportion of men also report modest changes in girth and, to a lesser extent, length. These P-shot before and after reports are the most variable and also the most commercially exploited claims online. Therefore, it is worth being clear about this. The primary mechanism of PRP is tissue health and vascular function. Any structural changes are secondary and not guaranteed.
Furthermore, men with organic erectile dysfunction — where the cause is genuinely vascular or nerve-related — may respond differently from men whose difficulties are largely psychogenic. A proper clinical assessment before treatment is essential.
Who Is a Suitable Candidate?
Not every man is an ideal candidate for the P shot UK clinics offer. A thorough assessment must come before any treatment decision.
Men who tend to respond well include those with mild to moderate erectile dysfunction, those experiencing reduced penile sensitivity with age, men who have completed treatment for prostate cancer and still carry residual erectile difficulties, and men who have not responded adequately to PDE5 inhibitors such as sildenafil or tadalafil.
By contrast, men with active blood disorders, those on anticoagulant therapy, or those with certain platelet function abnormalities may not be suitable. A clinician should review full medical history, current medications, and relevant blood work before proceeding.
Importantly, age alone is not a contraindication. Men in their 40s, 50s, 60s, and beyond have all taken part in clinical studies with positive outcomes.
The Procedure Itself: What to Expect
A clinician performs the procedure under local anaesthetic, and it typically takes under an hour in total. The clinician draws a blood sample from the patient’s arm — usually around 20 to 30 millilitres. A dedicated centrifuge then processes this sample for approximately 10 to 15 minutes. The centrifugation separates the blood into its components. Next, the clinician extracts the platelet-rich layer and prepares it for injection.
Before the injection, the clinician applies a topical and injectable local anaesthetic to the treatment area. The clinician then injects the PRP into the corpus cavernosum and, in some protocols, into the glans. As a result, patients typically report minimal discomfort during the procedure itself.
There is no significant downtime after treatment. Most men return to normal activity the same day. The treating clinician generally advises resuming sexual activity after a short period — typically a few days.
The full effect of the treatment builds over weeks. A single session is the starting point. Some men benefit from a second treatment three to six months later, though protocol varies by clinic and individual response.
Priapus Shot Price and What Drives the Cost

Priapus shot price varies across the UK, and it is worth understanding what goes into that cost. Male enlargement injections cost UK-wide typically range from £1,500 to £2,500 per session, depending on the clinic, the practitioner’s qualifications, and the equipment used.
Several components drive the cost. First, there is the laboratory processing — a dedicated centrifuge validated for PRP preparation is not cheap, and its maintenance directly affects quality control. Second, the clinical time involved includes consultation, assessment, the procedure itself, and follow-up. Third, the practitioner’s level of training and credentialing directly affects safety and outcome.
A low price point is not necessarily a reassurance. In fact, it may indicate corners being cut — in centrifuge quality, processing time, or clinical oversight. Equally, a high price is not automatically a mark of superior care. Instead, patients should look at practitioner qualifications, clinic governance, and whether a proper consultation precedes treatment.
The P shot UK market has grown rapidly. With that growth comes variation in quality. Therefore, due diligence matters.
How to Evaluate a Clinic
Choosing where to undergo this treatment deserves the same rigour anyone would apply to any medical procedure. Several questions are worth asking before booking.
Is the practitioner a licensed medical doctor? What is their specific training in sexual medicine or aesthetic plastic surgery? Does the clinic perform a full consultation and medical history review before treatment? Is the centrifuge CE-marked and validated for PRP preparation? Does the practitioner explain realistic outcomes — including the absence of guarantees?
At Pshots, Dr Syed Nadeem Abbas — holding MBBS, MRCS, MRCGP, and an MSc in Aesthetic Plastic Surgery with Distinction from Queen Mary University London — leads the clinical approach with training backgrounds from Cambridge, Oxford, and the Royal London Hospital. That level of credentials matters in a field where unregulated practitioners have unfortunately set up practice.
Ultimately, the priapus shot is a medical procedure. A medically qualified professional should deliver it in a proper medical setting.
Limitations and What the Evidence Does Not Yet Show
It would be misleading to present this treatment as a proven cure-all. The evidence base, while promising, has real limitations.
Most studies to date have been small — ranging from a few dozen to a few hundred participants. Moreover, few have used sham-injection control groups, which makes it harder to separate the placebo effect from genuine biological response. Long-term follow-up data beyond 18 months remains limited. Additionally, no standardised PRP preparation protocol exists, meaning the platelet concentrations that researchers use across different studies and clinics vary considerably.
NICE has not issued formal guidance specifically on PRP for erectile dysfunction. The NHS does not offer this procedure. That does not make it invalid — many effective interventions exist outside NHS provision — but it does mean patients are operating in a less regulated environment.
As a result, a responsible clinician will acknowledge these limitations openly. Anyone presentingpenile injection growth as certain, or quoting dramatic P shot before and after outcomes as standard, is overpromising.
A Final Word on Realistic Expectations

The science behind PRP therapy is sound. The biological rationale for its application in erectile tissue is coherent and early clinical data supports it. The safety profile is favourable. These are meaningful statements.
Nevertheless, the P Shot London patients seek is not a replacement for cardiovascular health, healthy weight, adequate sleep, and managing the conditions — diabetes, hypertension, high cholesterol — that most commonly underlie erectile dysfunction. Rather, it is a tool within a broader approach to male sexual health. Used appropriately, in the right patients, by the right clinicians, it offers genuine benefit.
Mark, from the opening of this article, went ahead with the treatment. He reported improvements in erectile quality at around eight weeks. Sensitivity improved. His confidence returned. He also lost a small amount of weight, stopped smoking, and started sleeping better. He attributes the change to all of it, not the injection alone. That is probably the most honest framing available.
Platelet-rich plasma therapy for sexual health sits at the intersection of established regenerative biology and an evolving evidence base — so given what we now understand about how PRP influences vascular tissue, how do you think the next decade of research will reshape how we approach age-related sexual decline in men?
read more: Understanding the Priapus Shot in London: A Game-Changer for Men’s Sexual Health
How the Priapus Shot in London Can Improve Your Relationship and Quality of Life